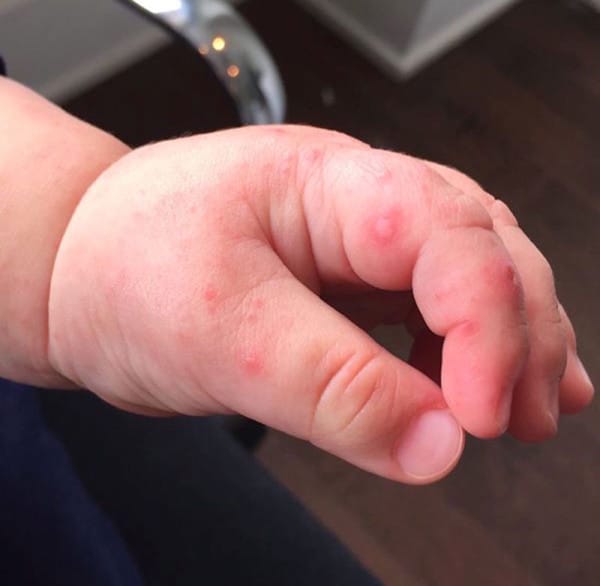
Small raised areas on your hands can be caused by various conditions. Blisters on the hands can present as clear bumps on fingers and even palms.
Skin rashes due to allergies or eczema (dyshidrotic eczema) can also produce a similar symptom, only that the size of the spots may be smaller.
- Depending on the cause, the lumps on your hands can be itchy or not itchy at all.
- Their color may also vary. Some are red due to inflammation.
- Infected bumps and pimples may appear white or yellowish.
- Sometimes fingerjoints may be affected especially if the cause is arthritis.
- Bumps between fingers, bacterial and fungal infections may be the reason for this.
When they are painful and itchy, they can produce a lot of discomfort and may need proper treatment to go away.
Here’s a picture for illustration of the symptom.
Causes
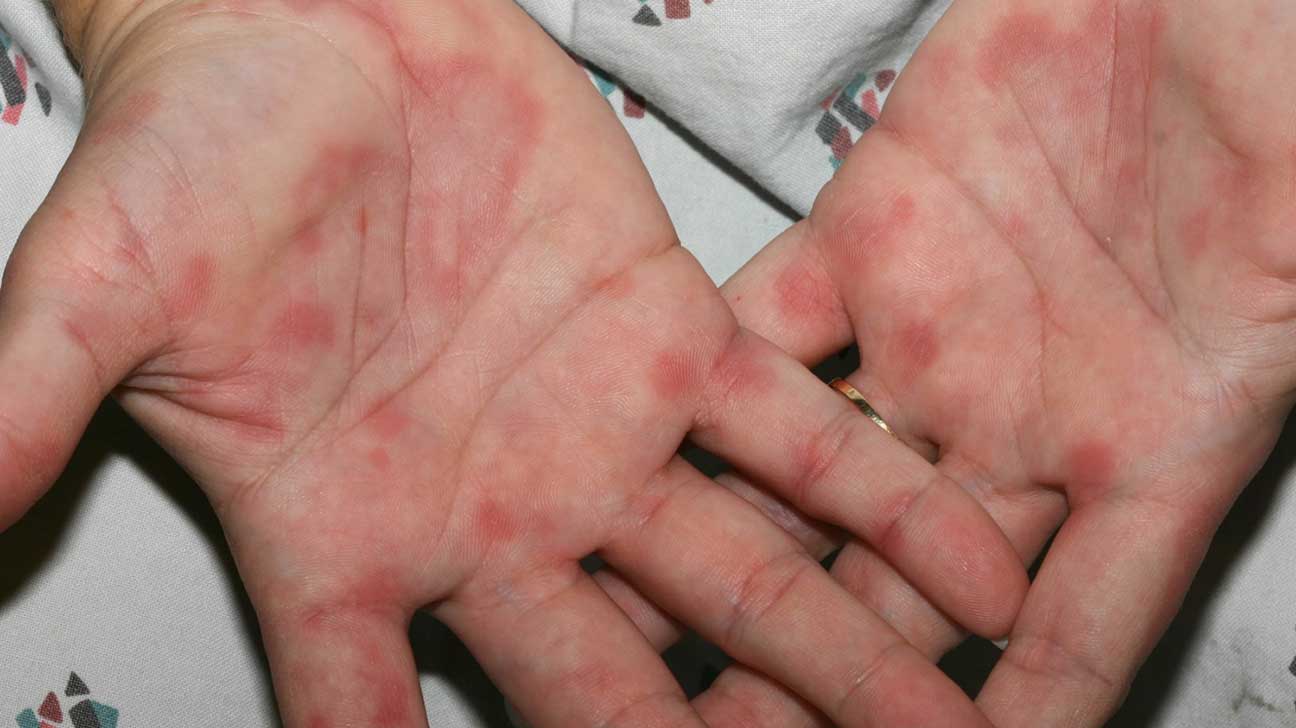
Dyshidrotic eczema is a skin condition where the blisters develop on the soles of the feet and the palms of the hands.
The bumps on fingers are normally itchy and can be filled with a fluid. Blisters usually last for about two to four weeks and can be related to the seasonal allergies or even stress.
A type of dermatitis, dyshidrotic eczema is more common amongst the women.
Dyshidrotic eczema, also called dyshidrosis is a type of eczema that leads to a blistering rash on the hands or feet, especially on the fingers, palms, and the soles.
The bumps on fingers are normally small and often itchy.
Dyshidrotic eczema is the third most common type of dermatitis, or inflammation, of the hands. It’s twice as common among the women as men.
About half of those who suffer from the dyshidrotic eczema also have the atopic dermatitis, which is a common form of eczema.
Dyshidrotic eczema is also a common side effect of the intravenous immunoglobulin infusions which are normally applied to treat certain immune system diseases.
The characteristic bumps on fingers of this condition includes:
- Small, similar to grains of the tapioca
- Filled using clear fluid
- In clusters between the fingers and toes or on the edges of the fingers, palms, or soles
- Very itchy and at times painful
The blisters normally dry and peel in about four weeks. The skin beneath them can be scaly, red, cracked, and also painful.
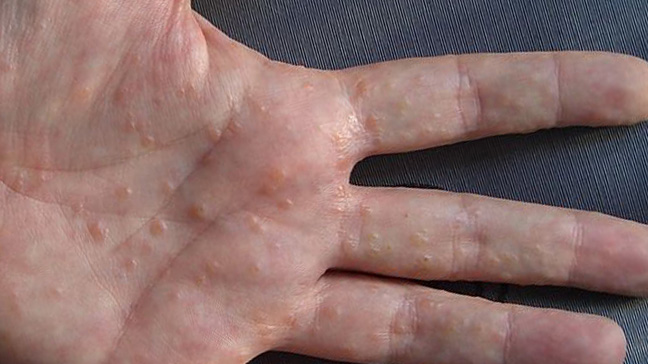
If you have dyshidrotic eczema, you may notice the blisters forming on the fingers, toes, hands, and feet. The blisters can be common on the edges of the areas and may probably be full of fluid. Sometimes, large blisters can form, which may be particularly painful.
The bumps on fingers can usually be very itchy and may cause the skin to flake. Some other people report that the affected areas become cracked and are painful to the touch.
The blisters may last up to a period of three weeks before they start to dry. As the blisters dry up, they’ll then turn into skin cracks that can be very painful. If you have been scratching the affected areas, you will also notice that the skin seems thicker or even feels spongy.
The cause of dyshidrotic eczema is much unknown, but more than one factor likely plays the role.
It can happen along with the atopic dermatitis or even hay fever, flaring seasonally together with any other allergies you may have.
Doctors understand that you have a greater chance of developing this condition if you’re having a high level of stress (which is either physical or emotional) or experience allergies. Some doctors also think that dyshidrotic eczema can be a type of allergic reaction.
A person can be more likely to get dyshidrotic eczema if the hands or feet are often moist or in water or if the work exposes you to the metal salts, such as cobalt and nickel.
About 50 percent of people with this skin condition are also troubled with the hands or feet that perspire too much.
Dyshidrotic eczema is very likely to occur if you:
- Are under a lot of stress
- Experiences atopic dermatitis
- Have sensitive skin in general
- Have allergies, including the hay fever
- Wash the hands frequently or your hands are often in water
- Work using cement
- Receive intravenous immunoglobulin infusions so as to treat another medical condition
In most of the cases, the doctor can be able to diagnose dyshidrotic eczema by examining of the skin carefully. Due to the symptoms of dyshidrotic eczema that can be similar to those of other skin conditions, the doctor can choose to run certain tests.
The tests include a skin biopsy that involves removal of a small patch of skin for lab testing. The biopsy may rule out other possible causes of the bumps on fingers, such as a fungal infection.
If the doctor believes that the outbreak of dyshidrotic eczema is very directly related to the allergies, they can also order allergy skin testing.
Bumps on fingers not itchy
Rheumatoid arthritis, is an autoimmune disorder that leads to the body’s immune system to attack the lining of the joints. It is twice more common in women than in men, and normally strikes between the ages of 50 and 60, although it may occur at any other age.
Doctors don’t know what leads to the disease, but the genes can make you more susceptible to it.
The disorder usually leads to the whole-body symptoms like fever and fatigue, but most of the damage the disorder causes is in the joints, especially the hands and the feet. The disorder gets rid of cartilage and bone in the joints and then loosens the tendons that hold the bones together.
If you have the disorder, there is about a 30 percent chance that can develop rheumatoid nodules pink or reddish bumps on or next to the affected joints that are firm, moveable and not painful.
Doctors don’t know what leads to the bumps, but they often indicate a more severe case of RA that requires more aggressive treatment.
When on finger joints
Dyshidrotic eczema, is a skin condition in which a small, fluid-filled blisters are shown on the palms of the hands and the sides of the fingers. The soles of the feet also may be affected.
Hand dermatitis is a very group of acute and chronic eczematous disorders that affects the dorsal and palmar aspects of the fingers.
Hand dermatitis is also called hand eczema
The bumps on fingers that happen in dyshidrosis usually last around four weeks and lead to intense itching. Once the blisters of dyshidrosis dry, the skin may appear very scaly. The blisters normally recur, sometimes before the skin heals completely from the previous blisters.
Treatment for dyshidrosis most usually includes creams or ointments that you rub on the affected skin. In severe cases, your doctor may suggest corticosteroid pills, such as prednisone, or injections.
Stress bumps on hands
Your emotions have a powerful effect on your skin. Since stress is a part of life, what matters is how you handle it.
Stress causes a chemical response in the body that makes the skin to be more sensitive and more reactive. It can also make it harder for skin problems to heal.
Have you ever noticed that when you are much stressed, you break out more. This is because stress leads to the body to produce cortisol and other hormones, which tells the sebaceous glands to produce more oil. Oily skin is more prone to bumps on fingers and other skin problems.
Are they painful?
Hand dermatitis can affect the backs of the hands, the palms or even both. It may be very itchy, often burns, and is sometimes more painful. It contains acute, relapsing and even chronic phases.
Acute hand dermatitis presents with the following:
- Red macules, papules and plaques
- Swelling
- Blistering and even weeping
- Fissuring
Features of chronic hand dermatitis are:
- Dryness and scale
- Lichenification
There are several causes and clinical presentations of hand dermatitis.
Atopic hand dermatitis depends on the constitutional weakness of the skin barrier function and is triggered by the contact with irritants. It can affect one or both of the dorsal hands and the palms. It might manifest as a discoid pattern of eczema. Patients can also have eczema in other sites including feet and hands.
The hands are usually the most common place for irritant contact dermatitis, and is normally due to wet work and repeated exposure to the low-grade irritants. The finger-webs are the first to be affected, but inflammation may extend to fingers, the backs of the hands as well as the wrists. Irritant contact dermatitis often spares the palms.
- Acute irritant dermatitis is due to the injury by potent irritants like the acids and alkalis, normally in an occupational setting.
- Repeated exposure to the low-grade irritants such as water, soaps, and detergents causes chronic cumulative irritant dermatitis.
Hard lumps
Small fluid-filled blisters known as the vesicles normally appear on the fingers, hands, and feet. They are most common along the edges of the fingers, toes, palms, and soles. These bumps on fingers can be very itchy. They also cause scaly patches of skin that flake or get red, cracked, and painful.
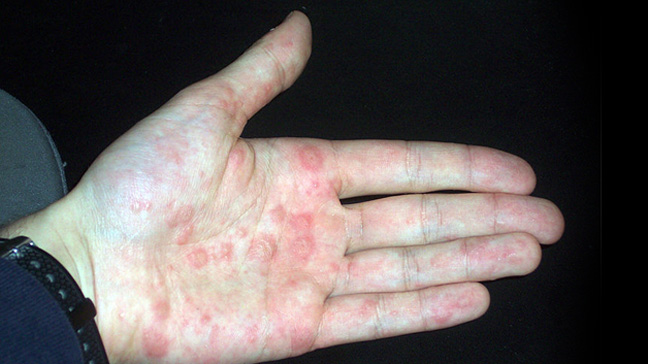
Scratching leads to skin changes and skin thickening. Large blisters may cause pain.
Granuloma annulare is a disorder that leads to the bumps or ring-shaped lesions on the skin, especially the hands, the feet, elbows or knees. The bumps are also red, purple, skin-colored or pearly white, and they can sometimes itch.
Most granuloma annulare bumps on fingers disappear on their own after a few months. No one knows what causes granuloma annulare, and treatment isn’t necessary unless you have a very severe case that causes cosmetic issues. If this is the case, the dermatologist will treat you with steroids or other medications or with ultraviolet light.
Small bumps
You use the hands for almost everything you do, so you will definitely notice if you develop red bumps on the finger joints.
Most of the conditions can lead to the bumps on the fingers; some are completely harmless, while others are very serious and need medical care.
If there’s no obvious lead to for the bumps, such as a bug bite or injury, or if the bumps don’t go away, see your physician to find out what is causing them.
Dermatomyositis is a muscle disease that leads to the chronic muscle inflammation and the weakness. A skin rash is the signature sign of this disease; the rash usually appears before the muscle symptoms.
The rash is normally purple or red and most often appears on the knuckles, eyelids, knees or even the toes, although it might appear on the back, face, chest or upper shoulders. Light will often make the rash or muscle symptoms worse.
There is no specific cure for dermatomyositis, but you have treatment options including corticosteroid drugs, heat therapy, physical therapy, assistive devices and rest the treatment the physician chooses for you depending on the type and severity of your symptoms.
Red bumps
Pompholyx is a type of eczema that leads to the tiny blisters to develop across the fingers, palms of the hands and at times the soles of the feet.
It’s also called dyshidrotic eczema.
Pompholyx may affect the people of any age, but it is most often observed in adults under the age of 40 years of age. Pompholyx normally starts as intense itching and burning of the skin on the hands and fingers. The palms and sides of the fingers (and sometimes the soles of the feet) then erupt into tiny itchy blisters that can weep fluid.
Small fluid-filled blisters known as vesicles appear on the fingers, hands, and feet. They are usually common along the edges of the fingers, palms, and soles. These blisters may be very itchy. They also lead to the scaly patches of skin that flake or get red, cracked, and painful.
Scratching causes the skin changes and skin thickening. Large blisters can lead to pain or can get infected.
In severe cases, the bumps on fingers can be quite large and can spread to the backs of the hands, feet and the limbs.
The skin may sometimes become much infected. Signs of an infection may include the blisters becoming very much painful and oozing pus or becoming covered in a golden crust.
The blisters will then heal within a few weeks. The skin also tends to become dry and crack or peel as it starts to heal.
It’s not clear exactly what leads to pompholyx, but it can be triggered by:
- a fungal skin infection – this may be on the hands or at a distant site from the blisters (such as in between the toes) and will need treating
- a reaction to something that has touched your skin – like thecertain metals detergents, household chemicals, soap, , cosmetic products or perfume
- stress
- sweating– pompholyx is more common in spring and summer, in warmer climates, and in people with hyperhidrosis
Lichen planus is also an inflammatory disease that leads to a rash of purplish-red flat-topped bumps that are very itchy. The rash appears on the skin, including the fingers, but more especially the wrists and ankles. Most of the dermatologists considers lichen planus an autoimmune disease; it is not very contagious.
You can also get lichen planus in the mouth or then develop ridges on the fingernails. The dermatologist will tell you if you have lichen planus and then prescribe a treatment such as topical corticosteroid cream, anti-inflammatory medication or even ultraviolet light treatment, depending on the severity of the symptoms.
How to get rid of them
In most of the cases, pompholyx can clear up on its own within very few weeks. The treatments of the doctor may help relieve the symptoms in the meantime.
Sometimes pompholyx may just happen once and may never come back, but it often comes and goes over several months or years. Any of the triggers mentioned above can cause it to flare up again.
Sometimes, pompholyx can be very continuous and thus difficult to treat
You should try to avoid any contact with anything that can irritate the skin, including soaps, shampoos and other household chemicals.
Use an emollient as a soap substitute and wear cotton-lined gloves when you’re at risk of contact with other potentially irritating substances, like when washing the hair or doing housework.
Don’t burst the bumps on fingers but rather you should let them heal on their own. If they’re particularly big, the doctor may be able to drain them.
The main treatments the doctor may recommend to treat the symptoms of pompholyx are same as those applied when treating atopic eczema, are:
- emollients – use these all the time and instead of soap to stop your skin becoming dry
- steroid cream– this reduces the inflammation and irritation and helps the skin to heal
Your the will probably prescribe a strong steroid cream to apply for a short period of time, to minimize risk of steroid side effects. You may be advised to wear cotton gloves at night to assist the cream sink into the skin.
If the bumps on fingers keeps returning or is severe and doesn’t get better with the above treatments, your doctor can refer you to a specialist in treating of the skin conditions (that is a dermatologist).
A dermatologist can recommend one of the following treatments:
- phototherapy – controlled exposure to ultraviolet (UV) light
- steroid tablets or very strong steroid cream
- immunosuppressant creams or ointments, such as pimecrolimus
- immunosuppressant tablets or capsules, such as ciclosporin
- alitretinoin capsules – medication that helps improve severe eczema affecting the hands when other treatments haven’t worked
The doctor may be able to diagnose this condition by looking at the skin.
A skin biopsy can be required to rule out any other causes, such as the fungal infection or psoriasis.
If the doctor thinks the condition is due to an allergic reaction, allergy testing (patch testing) may be done.
Keep the skin moist by lubricating or moisturizing of the the skin. Use ointments (such as petroleum jelly), creams, or lotions.
Moisturizers:
- Should be very free of alcohol, scents, dyes, fragrances, or other chemicals.
- Work best when they’re applied to skin that is wet or damp. After washing or bathing, pat the skin dry and then apply the moisturizer right away.
- May be applied at different times of the day. For the most part, you can apply these substances as often as you need to keep your skin soft.
Medicines that assist to relieve itching can be bought without any prescription.
- Take an anti-itch medicine before the bedtime if you scratch in your sleep.
- Some antihistamines cause little or no sleepiness. These include fexofenadine (Allegra), loratadine, cetirizine (Zyrtec)
- Others can make you sleepy, including diphenhydramine.
Your doctor may prescribe topical medicines. These are ointments or creams that are applied to the skin to relieve bumps on fingers. Types include:
- Corticosteroids, which calm swollen or inflamed skin
- Immunomodulators, which assists to keep the immune system from reacting very strongly
Follow instructions on how to use these medicines. Do not use more than you’re supposed to use.
If symptoms are very severe, you may require other treatments, like the:
- Corticosteroid pills
- Corticosteroid shots
- Phototherapy (ultraviolet light therapy)
References
- Dyshidrotic Eczema: http://www.healthline.com/health/dyshidrotic-eczema#Symptoms5
- Pompholyx (dyshidrotic eczema): http://www.nhs.uk/Conditions/pompholyx/Pages/Introduction.aspx
- Dyshidrotic eczema: https://www.nlm.nih.gov/medlineplus/ency/article/000832.htm