White bumps on skin can be itchy or non itchy. They may be caused by excessive sun exposure, trapped protein beneath the skin (for white bumps under skin), or viral infection such as HPV.
Here’s a list of causes of these painless dry white bumps on your skin and how to get rid of them with treatments and remedies at home.
Are little white bumps on my skin Fordyce spots? Are they caused by HPV? Are they fungal infection? Skin infections and problems can range from dry white bumps to hard raised white spots on the skin.
These could be caused by sun exposure or just about anything you may not be thinking of. Let’s start by knowing what they are.
What are they?
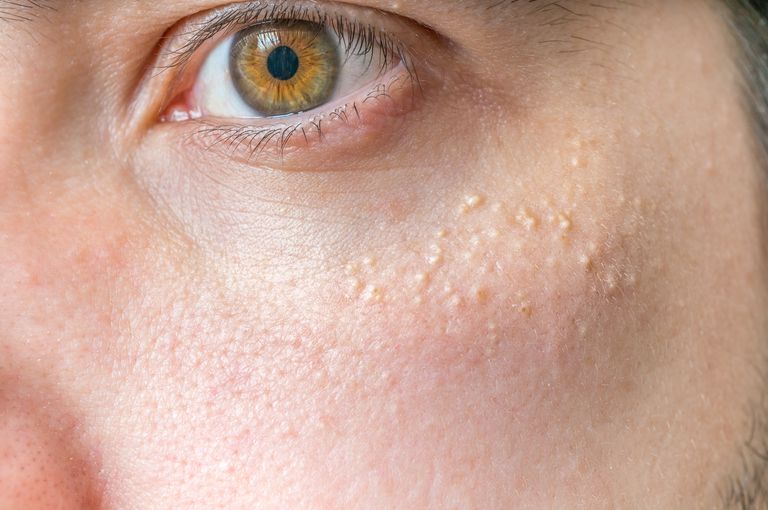
What are white bumps on skin? Such bumps may signal one of several things including viral infection (with molluscum contagiosum virus being the most common culprit), plugged pores leading to whiteheads, and thickening of the skin due to factors such as excessive sun exposure leading to the entrapment of dead skin cells beneath the surface layer of the skin.
RECOMMENDED FOR YOU:
- How to Get Rid of Pimple Marks
- Cluster of White Bumps on Lips Causes and Treatment
Understanding the symptoms associated with these underlying causes is critical to proper diagnosis and deciding the most appropriate intervention measures. We have discussed these causative factors in ore details in subsequent parts of this article.
Little White Bumps on Skin
Several skin conditions may be the underlying factors for those annoying little white bumps on skin including:
Milia: Milia are tiny harmless pearly-white bumps that typically occur on the nose, cheeks and around eyes even though they might as well appear anywhere on the body. They are typically filled with keratin, a type of protein.
Infants (babies aged below 1 year) are most susceptible to milia but older children and adults can as well suffer from the condition, with older women tending to get afflicted more commonly than other adults.
Milia are typically painless and are not bothersome. In fact most people only become aware of them from looking at the mirror. They look so much like, and are in fact commonly confused with acne whiteheads (discussed in the next section) but unlike whiteheads, milia are not surrounded by a rash (reddened skin).
Another notable difference between the two is that a milium is comprised of proteins that are trapped within the skin while a whitehead is comprised of sebum and dead skin cells that are trapped within skin pores.
How Milia Form
As the University of Maryland Medical Center says, milia occur when dead skin cells are entrapped beneath the outer layer of skin to form tiny cysts.
They typically form when the skin is not able to exfoliate – that is to slough off dead skin cells for replacement with new ones- effectively. This is often attributed to the use of heavy moisturizing lotions, cleansers, creams and other skin care products that trap dead skin cells.
Excessive sun exposure is also linked to the formation of milia. How exactly that happens is, however, still debatable As for milia occurring around the mouth, this is thought to be the result of irritation by fluoride in toothpastes.
A skin condition known as porphyria cutanea tarda is also known to cause milia. Porphyria cutanea tarda manifests itself in excessive hair growth on the hands and face and formation of blisters on the skin.
Genetics are also to blame for milia in some people. Yes, you could have inherited those milia from your parents.
Treatment of small milia spots
For children, milia typically go away in just a few weeks without any treatment as the Mayo clinic says.
Adults may however benefit from the following treatment options:
Use a deep cleanser: Washing your face with any brand of the deep cleansers out there may help to get rid of those white bumps (milia).
These cleansers are usually formulated for use on oily and blemish-prone skin types. They help to remove dirt and other environmental elements that may be responsible for clogging of sweat ducts, usually culminating in milia.
One brand that you may want to try is Germaine de Cappuccini Pure T. Your local beauty therapist may also be able to offer ou some recommendations.
Retinol creams: Applying retinol creams such as DERMAdoctor Poetry in Lotion 1% Retinol can also help to reduce the appearance of milia. An important point to note, however, is that retinol should not be used on the upper eyelids.
Surgical removal: A dermatologist can also remove those pesky milia cysts. This involves piercing the skin with a sterile needle while applying pressure to the surrounding tissue with a comedone extractor as to eventually make the cyst pop to the surface of the skin.
Exfoliation: Exfoliating the skin helps by keeping the epidermis layer of the skin thin and smooth which then encourage the sloughing off of dead skin cells – including those causing the and their replacement with new ones.
One effective way is microdermabrasion which is performed at a dermatologist’s office. This entails using a small ablative device to buff away the uppermost layer of skin and smooth out the cyst. Several sessions may be required for optimum results.
Your dermatologist may also decide to use chemical peels to remove the top layer of the skin to allow for regrowth of new healthy one that is free of milia. Several sessions of chemical peel treatment may also be needed for optimum results.
Caution: Do not try to remove milia at home as this carries the risk of infection particularly if the cysts are located on the eyelids.
Acne: Acne often results insmall white bumps on the skin called whiteheads. These are usually accompanied by a red rash unlike milia.
Acne tends to affect individuals with oily skin more. It starts with a build up of excess sebum – the oil produced in the skin. Sebum naturally makes its way to the surface of the skin through small openings in the skin called pores.
When produced in excess quantities, sebum often mixes with dead skin cells to clog the pores. As a result, a sebum-dead skin cells mixture gets trapped beneath the skin leading to formation of a microcomedone.
As it increases in size, it becomes a comedone which is either referred to as a white head or a blackhead depending on the color.
Whiteheads (often the culprits for white bumps) form when the pore is completely blocked by the sebum-dead skin cells mixture such that the comedone sits just beneath the surface of the skin.
Acne usually responds well to the following intervention measures:
- Applying over-the-counter creams and cleansers with benzoyl peroxide or salicylic acid
- Applying tea tree oil
- Stronger prescription topical creams – for severe persistent cases
- Oral antibiotics
Molluscum contagiosum: This is a contagious viral infection that causes a red rash coupled with one or more soft, smooth, wart-like red, skin colored or white bumps with a characteristic dimple-like indentation at the center.
The bumps can appear alone or in groups, rows, or clusters and tend to occur on the stomach, chest, arms, groin, legs, genital area, armpits, face and inner thighs (especially in sexually active adults and teenagers). The bumps can as well appear around the mouth and eyes but this is uncommon.
Molluscum contagiosum bumps are typically painless and heal on their own without necessitating treatment but they may in some cases become swollen, itchy, painful and infected.
The condition is caused by the Molluscum contagiosum virus and is most common among children aged between and 12 years even though teenagers and adults may as well be affected.
Athletes such as swimmers, boxers, wrestlers and gymnasts are also more prone to molluscum contagiosum and so are individuals with weakened immune system (e.g. those who have used steroids for a long time, have been infected with HIV, or are receiving cancer treatment).
The Molluscum contagiosum Virus (MCV) thrives in warm, humid climates as well as areas where people live in overcrowded conditions.
It is transmitted through small breaks in the skin when someone comes into contact with the skin of another infected person or with an infected object e.g. toys, towels, beddings etc. the virus can also spread in water which explains why swimmers are at higher risk.
The virus can also spread from one part of the body to another when an infected individual touch, or scratch the bumps and then touch another part of the body. It can also be transmitted sexually.
Although molluscum contagiosum bumps are usually small, they can grow to become as large as a pencil eraser or a pea in just a few weeks.
Getting rid of white spots on skin
Most cases of molluscum contagiosum will clear by themselves without any treatment. It takes between 2 and 3 months for each rash and bump to disappear but new ones tend to pop out as old ones heal which then makes some cases to take as much as 6 to 18 months to go away completely.
If deemed necessary there are numerous treatment options typically used to help with faster healing of the condition including:
- Using tweezers and scalpel to get rid of the contagious center
- Cryotherapy – freezing the bumps with liquid nitrogen
- Curettage – scraping the bumps off with a sharp instrument
- Creams containing salicylic acid, benzoyl peroxide, cantharidin, or tretinoin
- Prescription of an oral dose of cimetidine
Itchy white spots on skin
If you have white bumps on skin that itch, then molluscum contagiosum is one likely culprit. You will know if this common skin condition is to blame if the bumps have characteristic dimple-like centers.
Although non-itchy in most cases, molluscum contagiosum bumps may sometimes turn itchy. We have covered the molluscum contagiosum in more details in a previous section of this article.
If the skin also feels dry and has a sandpaper-like roughness, keratosis pilaris may be to blame. We have also covered it in another section of this article.
When under the skin
As for a whitish bump that feels to have a white dome that is more under the skin that on the surface of the skin, then you might be dealing with sebaceous cysts. So what are sebaceous cysts, you ask?
Well according to Medline Plus, a sebaceous cyst is a closed sac under the surface of the skin that may contain liquid or semi-liquid material. As a result, a cyst tends to move around when touched.
Sebaceous cysts are usually non-cancerous and tend to occur more commonly on the face, scalp, nape of your neck and trunk (especially the upper back). They grow slowly and are usually not a health concern unless they make you uncomfortable.
It might be a good idea however to have them checked by your doctor just to rule out cancer.
Placing a warm compress (a washcloth dampened with warm water) on the cysts may also help to drain the cysts and facilitate their healing according to the Medline Plus.
Your doctor may also decide to inject steroid medicine into the cysts to cut down on swelling. In some cases, surgery may be opted for to get rid of the cysts particularly if they are large or the patient has aesthetic concerns.
Dry and hard
As for those dry, hard white bumps on the skin that look like “goose-bumps”, keratosis pilaris may be to blame. This is a rather common skin disorder that affects the thighs and arms but may occur on any other part of the body including the face. The condition gives the skin a sandpaper-like feel.
The bumps usually result when a protein called keratin builds up in the skin as to cause hard plugs within the hair follicles. The bumps are usually painless but may in some cases get itchy.
Keratosis pilaris has a genetic aspect according to Medline Plus and tends to occur more commonly in people with very dry skin. It also tends to worsen in winter months when humidity levels take a dip.
Although keratosis pilaris clears away with time without requiring treatment, the following interventions may be used to alleviate the symptoms especially in patients with aesthetic concerns including:
- Keeping the skin moisturized with a good lotion
- Applying skin creams containing urea, salicylic acid, tretinoin, vitamin D, or lactic acid
- Steroid creams
Sun exposure
Those white bumps on skin may also be the result of prolonged sun damage. Sun causes skin aging which is marked by significant thickening of the epidermis. The thicker skin that results is then more prone to milia since it makes it more difficult for skin cells to find their way out of the glands.
Some studies have also linked milia and the resulting bumps to the active ingredient sunscreens the likes of Parsol 1789 which may result in sun allergies that eventually cause milia. Other studies have showed that the sun is directly to blame.
References
- Derma Doctor: Milia causes and treatments
- MedicineNet: How to get rid of Bumps on Skin
- National Health Service (UK): Keratosis pilaris (“chicken skin”)
